Medical aid in dying is a medical practice within the full spectrum of end-of-life care, including curative treatment, hospice, palliative care, pain management, the choice to refuse treatment, and voluntarily stopping eating and drinking. Even so, many people facing a terminal diagnosis are unsure how to use the option. Medical aid in dying is authorized in jurisdictions across the country, but the actual steps — such as how the process works and what the recent policy changes to expand availability mean — are not always clear. This guide breaks down the process so patients and families can understand what access looks like today.
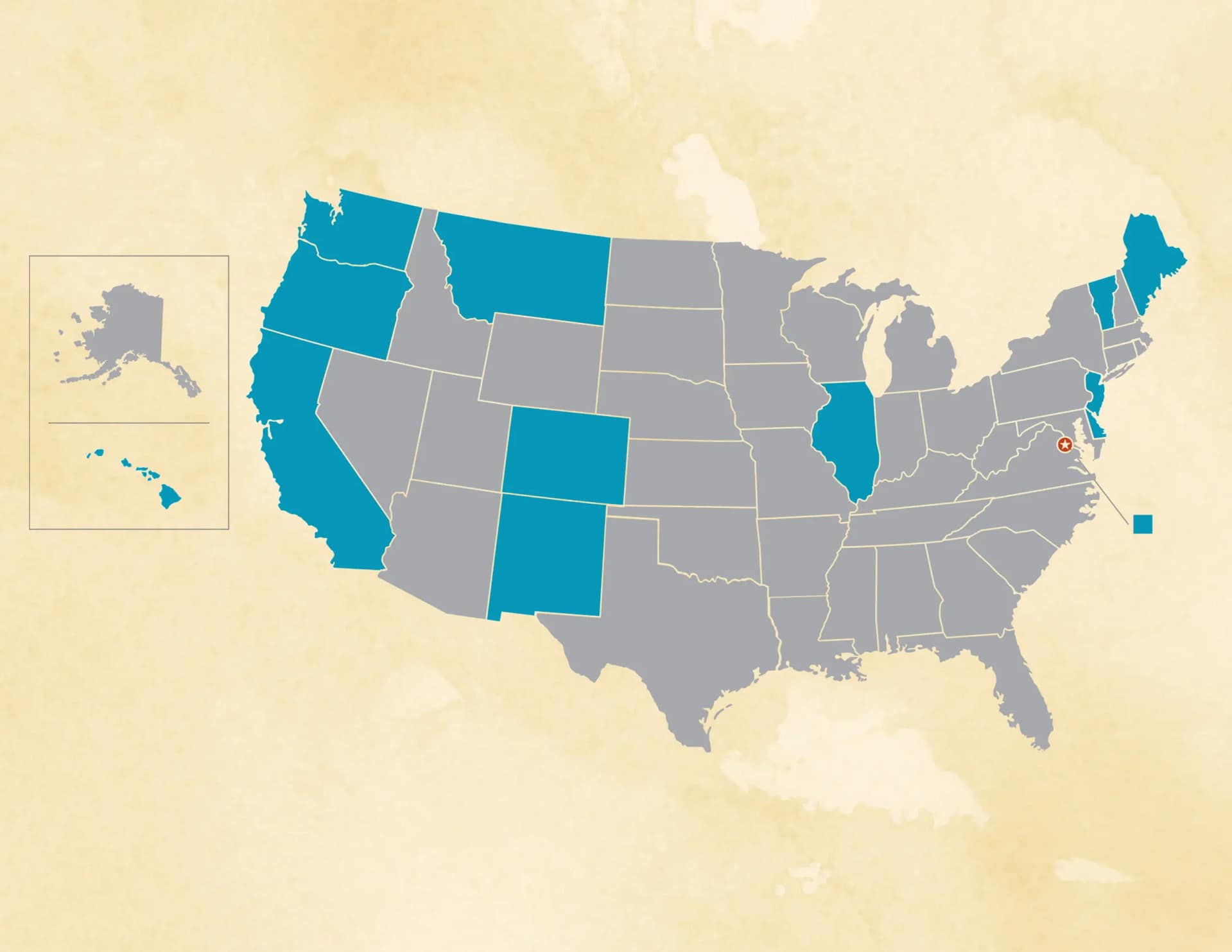
Medical aid in dying allows a terminally ill, mentally capable adult to voluntarily request and receive prescription medication from a healthcare provider that they can self-administer to die peacefully, on their own terms. Medical aid in dying is currently authorized in 14 U.S. jurisdictions: California, Colorado, Delaware, Hawai‘i, Illinois, Maine, Montana, New Jersey, New Mexico, New York, Oregon, Vermont, Washington state, and Washington, D.C. Every law* includes strict eligibility and safeguard requirements. To be eligible, an individual must:

Across authorized jurisdictions, the process follows the same core steps, even though timelines vary. A healthcare provider first confirms that the person has a terminal illness with a prognosis of six months or less to live and that the condition is incurable and irreversible. One or more healthcare providers, depending on the jurisdiction, verify that the patient has the mental capacity to understand information, weigh options, and communicate a choice; if there are concerns, a mental health evaluation is required.
Most laws require at least two verbal requests and one written request for the medication, made directly by the patient, and many include a waiting period between the verbal requests. The written request must be witnessed by one or more adults who attest that it is voluntary and free of coercion. Providers must also review all end-of-life care options, including comfort care, hospice, pain management, and palliative care.
When and if the person chooses to proceed, they may receive a prescription that they can choose to fill and self-administer. Participation is always voluntary; a patient may change their mind at any point, and no medical provider, institution, or individual is required to participate.
For many years, residency restrictions meant that only people who could prove they lived in an authorized state could access its law. That is changing state by state.
Vermont and Oregon have now permanently removed residency requirements, allowing eligible patients from other states to seek care there. At the same time, new laws continue to emerge. In 2025, Delaware authorized medical aid in dying with access beginning in January 2026. Illinois followed suit after Governor Pritzker signed the End-of-Life Options for Terminally Ill Patients Act (SB 1950) into law in December 2025; access will begin in September 2026.

Medical aid in dying allowed my wife to end her physical suffering and cross into the next life the way she wanted, on her own terms, with grace.
In March 2023, Rod Azama traveled with his wife, Susan, from Maryland to Oregon so she could access medical aid in dying after her incurable stage 4 cancer caused unbearable pain. Because the option was not authorized in Maryland, Susan could not spend her final moments at home with her dog, friends, and family nearby. Instead, Rod held her hand alone in a quiet rental far from everything familiar. Susan, a former NASA database specialist and devoted animal lover, chose the care that gave her comfort after learning she had only months to live.
When her pain became overwhelming despite hospice care, she took the prescribed medication and died peacefully with Rod beside her. Rod shared, “Medical aid in dying allowed my wife to end her physical suffering and cross into the next life the way she wanted, on her own terms, with grace. But she shouldn’t have had to travel out of state to do it.” Susan’s story is one of many that show why expanded access matters, so no one facing the end of life has to leave home, loved ones, or community behind to find peace.
Start the conversation. Talk with your healthcare provider and someone you trust about what matters most to you at the end of life, including whether medical aid in dying is an option where you live or where you would be able to travel. These conversations are an important first step in ensuring your wishes are known and respected.
We are here for you, and with your support we are building a future where everyone can access compassionate, patient-directed end-of-life care. Through education, advocacy, and direct support, Compassion & Choices advances a national access strategy that puts people first. You can be part of this effort by donating or volunteering to support our access strategy, legal work, and state-level campaigns. It is only with your support that change can be achieved.
If you are struggling to get the care you want and deserve, we are here to help. Call Compassion offers confidential support to help you get prepared, make a plan, or navigate challenges accessing care: 800.247.7421
Mail contributions directly to:
Compassion & Choices Gift Processing Center
PO Box 485
Etna, NH 03750
Compassion & Choices is a 501 C3 organization. Federal tax number: 84-1328829