Storyteller Spotlight: Trisha White
D.C. resident Trisha White, while grateful to have legal access to medical aid in dying, knows that practical access is not as straightforward and wants to help change that.
Feb 21, 2020
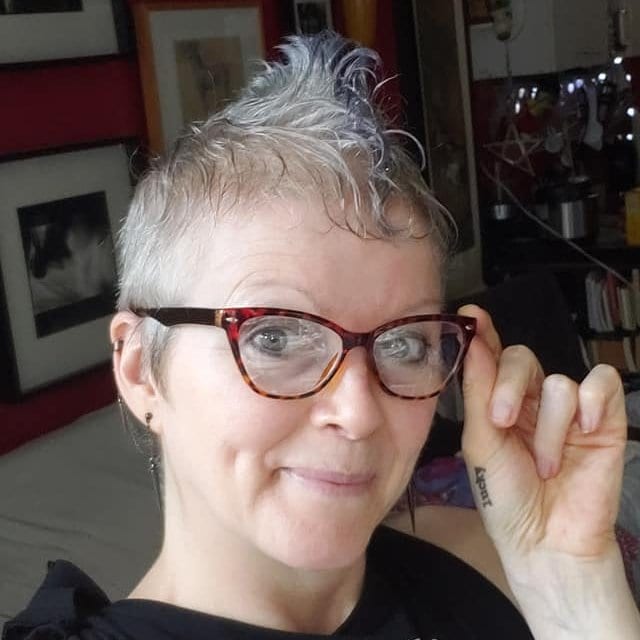 In 2011, after years of health challenges and with the blessing of his family, Trisha White’s father chose to end his suffering by voluntarily stopping eating and drinking (VSED). Because medical aid in dying is not available in his home state of Michigan, VSED was his only option. “We stayed by his side, hoping it would be peaceful, swift and merciful,” says Trisha, who lives in Washington, D.C. “It was not. Even at 86 years old, underweight and in poor health, it took him three weeks to die: three weeks in agonizing pain, in and out of consciousness and begging for death. By the time I left the farm after he died, my mourning was eclipsed by anger that my dad had to die like that. He deserved better, and we were unable to give it to him.” This painful experience reinforced Trisha’s belief that people deserve access to humane end-of-life options and strengthened her resolve to help make that a reality.
In 2011, after years of health challenges and with the blessing of his family, Trisha White’s father chose to end his suffering by voluntarily stopping eating and drinking (VSED). Because medical aid in dying is not available in his home state of Michigan, VSED was his only option. “We stayed by his side, hoping it would be peaceful, swift and merciful,” says Trisha, who lives in Washington, D.C. “It was not. Even at 86 years old, underweight and in poor health, it took him three weeks to die: three weeks in agonizing pain, in and out of consciousness and begging for death. By the time I left the farm after he died, my mourning was eclipsed by anger that my dad had to die like that. He deserved better, and we were unable to give it to him.” This painful experience reinforced Trisha’s belief that people deserve access to humane end-of-life options and strengthened her resolve to help make that a reality.
Seven years later — two months before her 50th birthday — Trisha noticed a lump in her right breast. After a barrage of scans, tests and biopsies, she learned it was stage four metastatic breast cancer, treatable but not curable. She began aggressive treatment: five months of chemo to shrink the lime-sized lump before a double mastectomy and six weeks of daily radiation.
“No one tells you that the hardest part of having terminal cancer is hurting people that you love; telling them your diagnosis and watching them cry,” says Trisha. “Now that I’ve completed treatment, I can honestly say it’s the easiest thing about having terminal cancer. It’s the thing we know how to do. We’ve all seen it in movies and TV shows; we know someone who’s been through it. We know the drill: show up, do the thing, get the needle, get the knife. Go home, puke, rest, recover, repeat. People bring you food and cheer you on. You’re an inspiration. But then what? What about the stuff we don’t know how to do, the stuff we don’t talk about because it’s too scary? What do we do with people when we don’t have a cure and we don’t have another treatment?”
Trisha is glad that with a new drug, a cancer that would have killed her in two years can now be held off for as many as 10. Still she acknowledges that medical technology can be a double-edged sword. “Science could have kept my dad alive for much longer. But at what cost? He understood the difference between quantity and quality of life.”
Unlike her father, she lives in a jurisdiction where medical aid in dying is legal. Yet, she’s aware that accessing the option is not easy. “The topic of medical aid in dying is still awfully scary, controversial and messy for some,” she says. “In my conversations with some well-meaning — albeit misinformed — people, I learned that fear of abuse can override sympathy for the dying. Some doctors and pharmacists are hesitant to be providers out of fear they will be labeled as ‘death doctors.’”
So Trisha is sharing her experience to help further the end-of-life choice movement while she’s able. “Changing the law was just the first step. Changing hearts and minds is up to us,” she says. “I couldn’t help my dad, but maybe I can help yours.”


